Highlights from the 2017 ISHRS (International Society of Hair Restoration Surgery) Scientific Meeting in Prague
 In October of 2017, the International Society of Hair Restoration Surgery (ISHRS) held its annual scientific meeting in Czech Republic. The annual meeting brings together many of the world’s leading hair transplant surgeons and hair loss researchers to discuss advancements in medical and surgical hair restoration.
In October of 2017, the International Society of Hair Restoration Surgery (ISHRS) held its annual scientific meeting in Czech Republic. The annual meeting brings together many of the world’s leading hair transplant surgeons and hair loss researchers to discuss advancements in medical and surgical hair restoration.
Background on the ISHRS
The International Society of Hair Restoration Surgery (ISHRS) is the most prominent professional organization for hair restoration in the world. Their primary mission is to educate hair surgeons ranging from the novice to the expert. Their website (http://www.ishrs.org/) provides useful information about hair restoration and profiles and contact information for its hundreds of worldwide physician members.
At the meeting, Dr. Sungjoo (Tommy) Hwang replaced Dr. Ken J. Washenik as ISHRS President for the coming year. Congratulations to Dr. Hwang for receiving this high honor. Coalition hair restoration physician Dr. Arthur Tykocinski was also named as Vice President.
Physician Recognition and Awards
Congratulations to the following award recipients:
Coalition hair transplant surgeon Dr. Jean Devroye of Belgium won the coveted Platinum Follicle Award for outstanding achievements in basic science and clinically-related research in hair pathophysiology and anatomy.
Dr. Edwin S. Epstein MD was awarded the Golden Follicle Award for his role in developing innovative hair restoration techniques and furthering the advancement of hair restoration.
This year, the Distinguished Assistant Award went to Anne Knudsen, RN of Sydney, Australia.
There was no Manfred Lucas Award winner for 2017.
Presentations of Interest to Hair Loss Sufferers
Below are the highlights of the exciting presentations from our recommended and Coalition physicians – and other hair loss experts – at the 2017 ISHRS conference:
The Benefits of a Two Person Team When Performing Follicular Unit Extraction (FUE)
 The success of any hair transplant surgery hinges on the survival of the follicular unit grafts that are harvested and subsequently implanted to the balding areas of the scalp. This is of particular concern with follicular unit extraction (FUE) due to several factors including the forces required to punch and extract the donor grafts as well as the slow and tedious nature of the process. Though FUE tools, techniques and procedures have continued to advance over the last few years, session sizes are typically smaller on average than strip surgery. However, recommended hair transplant surgeon Dr. Mike Vories of South Carolina has devised a protocol for performing FUE that allows him to extract and place up to 3000 FUE grafts in a single session.
The success of any hair transplant surgery hinges on the survival of the follicular unit grafts that are harvested and subsequently implanted to the balding areas of the scalp. This is of particular concern with follicular unit extraction (FUE) due to several factors including the forces required to punch and extract the donor grafts as well as the slow and tedious nature of the process. Though FUE tools, techniques and procedures have continued to advance over the last few years, session sizes are typically smaller on average than strip surgery. However, recommended hair transplant surgeon Dr. Mike Vories of South Carolina has devised a protocol for performing FUE that allows him to extract and place up to 3000 FUE grafts in a single session.
Dr. Vories is one of the few hair restoration physicians that participates in every aspect of the surgery from extraction to placing the grafts. Because removing and placing grafts up to 3000 per day demands efficiency, Dr. Vories’ protocol involves one surgical assistant and one physician to both extract tissue and place tissue. Over a two year period, he has steadily increased his daily graft number to finish an FUE procedure of 3000 grafts in a 9 hour procedure.
Materials and Methods

Graft extraction for a 3000 graft FUE case begins at 7:30 AM. Dr. Vories uses a Cole Instrument surrounded sharp punch with motorized rotation. Dr. Vories scores 100 grafts per pass and then removes the tissue with inverted curved forceps. With practice, he has been able to consistently harvest tissue at a rate of 750 grafts per hour, including a 15 minute break each hour. During this time the surgical assistant is counting and collating the grafts, and filling out a grid indicating the absolute hair count. By 12:00 PM they are ready to begin implantation.
Graft placement is performed using the Hans Lion Implanter. This process begins with the surgical assistant loading the implanter pens and the physician placing the grafts into a pre-designed grid using the “stick and place” method. No pre-made incisions are made. Inmost cases, four implanter pens are used at a time allowing for efficient placement of 500 grafts per hour with a 15 minute break per hour. Placement is typically finished by 6 PM.
Conclusion
Although this method is demanding, Dr. Vories believes there are multiple advantages to this approach that benefit both the patients and the surgical teams, including:
- Overhead is very low which allows the clinic perform just one procedure per day.
- The physician is in total control of the procedure, so quality control of the procedure is easily obtained.
- Patients desire the physician be directly involved with the procedure.
Measuring FUE Donor Capacity to Avoid Over Harvesting
 Over harvesting grafts from the FUE hair transplant donor area can lead to a see-through and “moth-eaten” appearance. In order to avoid this problem, recommended hair transplant surgeon Dr. James Harris of Colorado presented a study applying a measurement called Hair Mass Index (HMI) to aid surgeons in the proper management of the donor supply.
Over harvesting grafts from the FUE hair transplant donor area can lead to a see-through and “moth-eaten” appearance. In order to avoid this problem, recommended hair transplant surgeon Dr. James Harris of Colorado presented a study applying a measurement called Hair Mass Index (HMI) to aid surgeons in the proper management of the donor supply.
Hair Mass Index is an accurate measurement that allows the surgeon to calculate the volume, density and diameter of hair follicles in the permanent donor zone. HMI is expressed as mm2 of hair per cm2 of the scalp. Post-operative donor area HMI values of 29-32 yield a noticeable depletion and values of 20-24 result in an unacceptable depletion of the donor area.
Method
A test area in the mid occipital region of a test subject with no hair loss was identified. A region of 1.5cm x 1.5cm was shaved to a hair length of 1.5mm. A photograph with a Dermlite dermatoscope was obtained for determination of the number of follicular units/cm2 (FU density). A dermatoscope was used to obtain an estimate of the follicular unit density. Immediately inferior to this site, an area measuring 6cm in the lateral dimension and 1cm tall was marked. The lateral 2cm regions were used as controls, the center 2cm segment was identified as the test area. HMI of each of the three 2cm segments was obtained in the usual fashion using the “tare” method described by Dr. Bernie Cohen for HMI values less than 40 and recorded.
 Hairs associated with 5 discrete, randomly distributed follicular units were then trimmed to the scalp from the test area and then the test area HMI was obtained, the value recorded, and photographs taken. This process was repeated until the test area less than 20 signifying significant depletion.
Hairs associated with 5 discrete, randomly distributed follicular units were then trimmed to the scalp from the test area and then the test area HMI was obtained, the value recorded, and photographs taken. This process was repeated until the test area less than 20 signifying significant depletion.
Results and Analysis
The investigator evaluated the photos and a subjective evaluation of “noticeable” and “unacceptable” depletion was made for each subject. “Noticeable” depletion was noted in all subjects when the HMI reached 29-32 and “unacceptable” depletion was noted at an HMI of 20-24.
The HMI/follicular unit was calculated for each successive group of five follicular units trimmed in each patient to create a model whereby a physician can input the starting HMI and the calculated HMI/FU and obtain the number of follicular units that could be removed to obtain a noticeable. The results to date suggest that this may be possible but additional subjects are needed.
To date, 7 subjects have been enrolled in the study with plans for at least an additional 5 subjects. The range of initial HMI’s was 18-51 and the range of FU density was 73-111.
Conclusion
This study will provide guidelines for physicians performing FUE on how to assess and pre-operatively judge donor area capacity and guide decisions about safe extraction limits.
Sexual Dysfunction Among Propecia (Finasteride) Users
 Concerns about the incidence of erectile dysfunction and libido loss among Propecia (finasteride) users remains high, and the existence of post finasteride syndrome remains controversial. Coalition hair restoration physician Dr. Robert Haber gathered sexual function data from finasteride using males as well as non-using controls from his clinic patient population, established a baseline sexual function among non-users, and compared this baseline to finasteride users, in order to help determine if finasteride use was correlated with sexual function.
Concerns about the incidence of erectile dysfunction and libido loss among Propecia (finasteride) users remains high, and the existence of post finasteride syndrome remains controversial. Coalition hair restoration physician Dr. Robert Haber gathered sexual function data from finasteride using males as well as non-using controls from his clinic patient population, established a baseline sexual function among non-users, and compared this baseline to finasteride users, in order to help determine if finasteride use was correlated with sexual function.
Method
In this office based population study, adult male patients visiting Dr. Haber’s office for any reason between August 2013 and January 2017 were asked to complete a sex survey. Finasteride users completed a survey that included a modified Arizona Sexual Experiences Scale (ASEX) as well as specific questions related to duration of finasteride use, alcohol use, and actions taken if sexual dysfunction was reported. Non-finasteride users completed the same questionnaire, but without finasteride specific questions. Over 800 questionnaires were completed and data were analyzed to determine comparative incidence of ED and libido loss among finasteride users and age matched controls.
Conclusion
Surprisingly, the results support the conclusion that finasteride use is not associated with an increased risk of sexual dysfunction. The overall prevalence of sexual dysfunction in the control group was 26%, while the overall prevalence of sexual dysfunction in the finasteride using group was 27%. Notably, the modified Arizona Sexual Experiences Scale (ASEX) results revealed a greater degree of sexual dysfunction in all age groups other than 40-49. A more complete data analysis will be presented as well as plans for follow-up studies.
A New Method of Quality Control in Hair Restoration Surgery
 Graft quality is extremely important to the success of a hair transplant. FUE grafts are often characterized as having lower yield than microscopically dissected grafts produced in strip surgery. Grafts of high quality have supportive tissue throughout, and contain minimal transections, follicle fractures and crushed follicles. Transections and stripped follicles are byproducts of punch insertion technique. Follicle fractures and crushes are byproducts of the amount and type of force used to remove the grafts once they have been punched. High quality grafts are easy to place without undue manipulation or placement trauma.
Graft quality is extremely important to the success of a hair transplant. FUE grafts are often characterized as having lower yield than microscopically dissected grafts produced in strip surgery. Grafts of high quality have supportive tissue throughout, and contain minimal transections, follicle fractures and crushed follicles. Transections and stripped follicles are byproducts of punch insertion technique. Follicle fractures and crushes are byproducts of the amount and type of force used to remove the grafts once they have been punched. High quality grafts are easy to place without undue manipulation or placement trauma.
In the following study, Coalition hair transplant surgeon Dr. Robert True introduces the concept of a Graft Placement Index (GPI) and proposes that this index can be used in all surgeries, whether strip or FUE, to grade and predict the difficulty of graft placement. GPI has four grades with Grade 1 being the easiest to place and Grade 4 the most difficult.
Grade 1 – Grafts have no protruding transections, a smooth regular border, perifollicular tissue throughout the follicle length, and non-follicular tissue to grasp for forceps insertion.
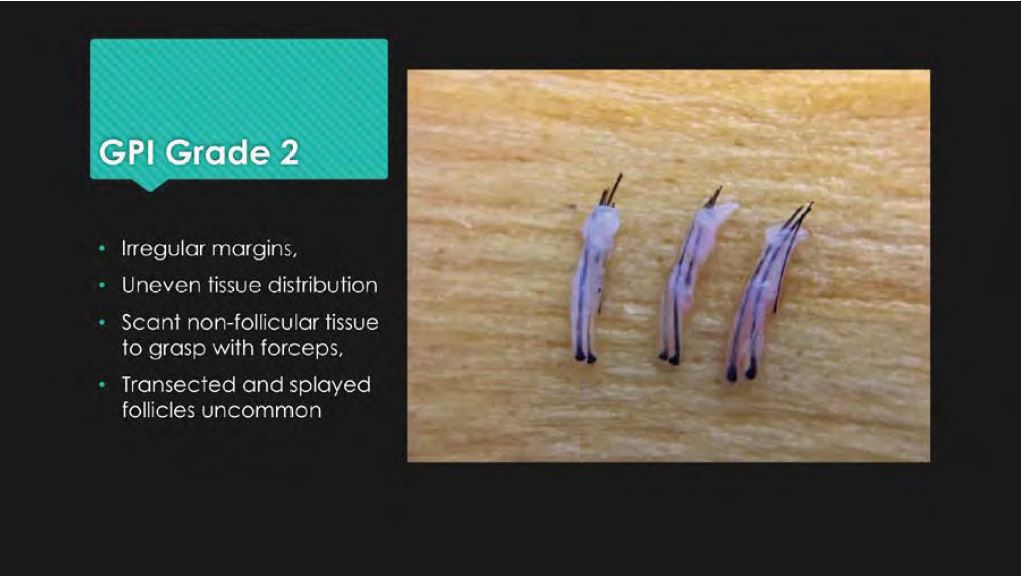
 Grade 2 – Grafts have irregular margins and uneven tissue distribution and not tissue to grasp with forceps,
Grade 2 – Grafts have irregular margins and uneven tissue distribution and not tissue to grasp with forceps,
protruding splayed or transected follicles are uncommon.
 Grade 3 – Grafts have irregular margins, and may contain some splayed follicles, transected follicle shafts and naked bulbs.
Grade 3 – Grafts have irregular margins, and may contain some splayed follicles, transected follicle shafts and naked bulbs.
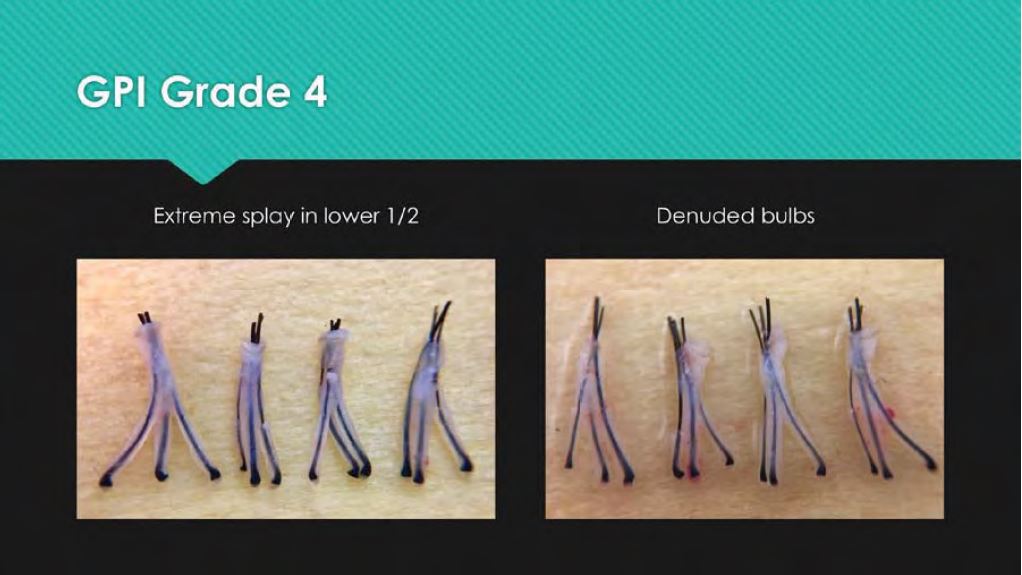
 Grade 4 – Grafts have extreme splay with the lower half to 1/3 of the follicles being denuded of surrounding tissue and contain partial transections with protruding portions of follicle shafts.
Grade 4 – Grafts have extreme splay with the lower half to 1/3 of the follicles being denuded of surrounding tissue and contain partial transections with protruding portions of follicle shafts.
Conclusion
Dr. True believes that Grades 1 and 2 will have minimal placement trauma when using forceps for placement. However, Grades 3 and 4 will have less placement trauma when using implanters.
Advances In Hair Cloning
 Today’s state-of-the-art hair transplant surgery can produce extremely natural and undetectable results. However, the patient’s limited supply of DHT resistant donor hair means that full, natural density cannot be truly replicated. One long-awaited solution to this problem is hair cloning. The ability to multiply hair follicles through cloning has the potential to enhance or even replace hair transplantation in the future.
Today’s state-of-the-art hair transplant surgery can produce extremely natural and undetectable results. However, the patient’s limited supply of DHT resistant donor hair means that full, natural density cannot be truly replicated. One long-awaited solution to this problem is hair cloning. The ability to multiply hair follicles through cloning has the potential to enhance or even replace hair transplantation in the future.
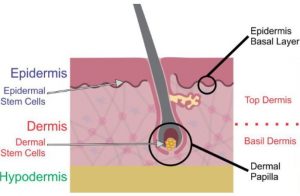
Tissue engineering lecturer Dr. Claire Higgins, PhD of Imperial College London, discussed advances in hair cloning using adult dermal papillae from hair follicles to induce growth of an entirely new follicle. Adult dermal papillae retain the embryonic property of inductivity. During skin development, condensation of dermal cells underneath the epidermis stimulates overlying cells to differentiate and form the hair follicle. Epidermal cells eventually engulf the dermal condensate forming the dermal papilla, which, if excised and implanted into non-hair bearing skin has the ability to induce new hair follicle growth. Thus, the adult dermal papilla retains the embryonic property of inductivity. This property is the basis of the science behind hair follicle cloning, i.e. the idea that an adult dermal papilla from a hair follicle can be used to induce growth of an entirely new hair follicle.
One problem arises when dermal papilla cells are grown in vitro; they quickly lose their ability to induce new hair follicle growth. Thus, research is focusing on ways to improve the hair inducing capacity of dermal papilla cells in culture. We and others have previously demonstrated that one way to restore inductivity is by forcing dermal papilla cells to aggregate, effectively, reprogramming them by promoting condensation. We are currently trying to decipher how nuclear architecture and transcriptional activity is affected by condensation, to understand how aggregating dermal papilla cells results in increased inductivity.
Research is focusing on ways to improve the hair inducing capacity of dermal papilla cells in culture. Dr. Higgins and others have previously demonstrated that one way to restore inductivity is by forcing dermal papilla cells to aggregate, effectively, reprogramming them by promoting condensation. They are currently trying to decipher how nuclear architecture and transcriptional activity is affected by condensation, to understand how aggregating dermal papilla cells results in increased inductivity.
Regenerating Transected Hair Follicles in the Hair Transplant Donor Area Using FUE
Transection is the act of unintentionally severing the hair follicle during harvesting of the donor hair. This is of most concern with follicular unit extraction (FUE) as the natural hair groupings are scored with very small punches, leaving little room for error. These follicles can be either completely transected, when all of its follicles are cut transversely, or partially transected when one or more follicles are cut leaving one or more follicles intact.
The opinion of some FUE hair surgeons that the transection rate is not important because the transected follicles will regrow is not generally accepted. Similarly, they believe that grafts that are purposely transected in vivo survive and continue to grow, whereas the remaining split grafts in the donor area also regenerate at high rates.
A study performed by Coalition hair transplant surgeon Dr. Jean Devroye of Belgium, claimed that only 60% of the transected follicles regrow. Furthermore, the regrowth is unpredictable and is more likely if the transection occurs at the upper part of the follicle. The purpose of the following study by Dr. Georgios Zontosis is to precisely quantify the regrowth rate of the transected hair follicles by using advanced imaging processing techniques.
Materials and Methods
The researchers transected the follicular units both totally and partially to simulate real surgical conditions. In addition, the areas of interest in the donor region were permanently marked by a tattoo. Specifically, the study involved 8 areas from 3 patients. Each area was tattooed using a permanent pigmentation. Black dots were made at the corners at each square. (Fig 1,2,3) The surface of each square was approximately 0,33 mm2 in order to match with the optical field of a USB micro camera.
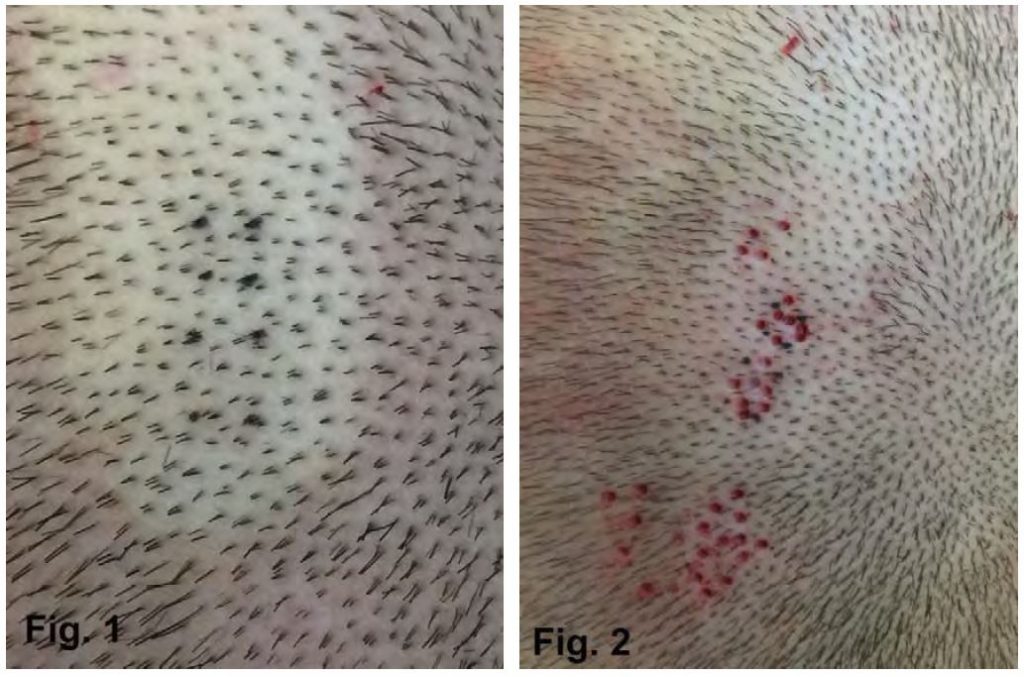
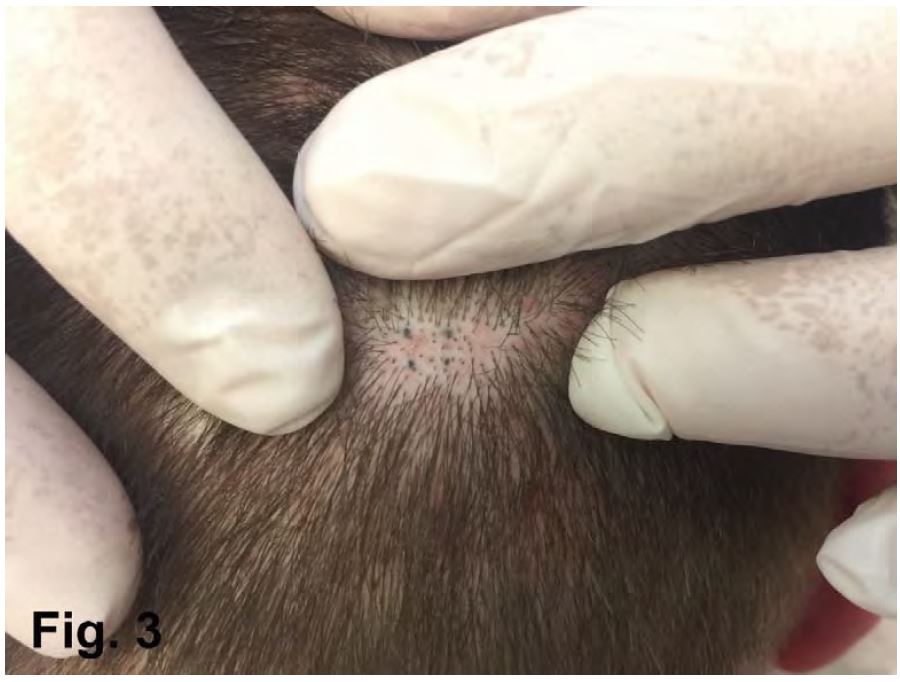 Macro and micro photographs were taken of each square before and after the harvesting process and 7 months later.
Macro and micro photographs were taken of each square before and after the harvesting process and 7 months later.
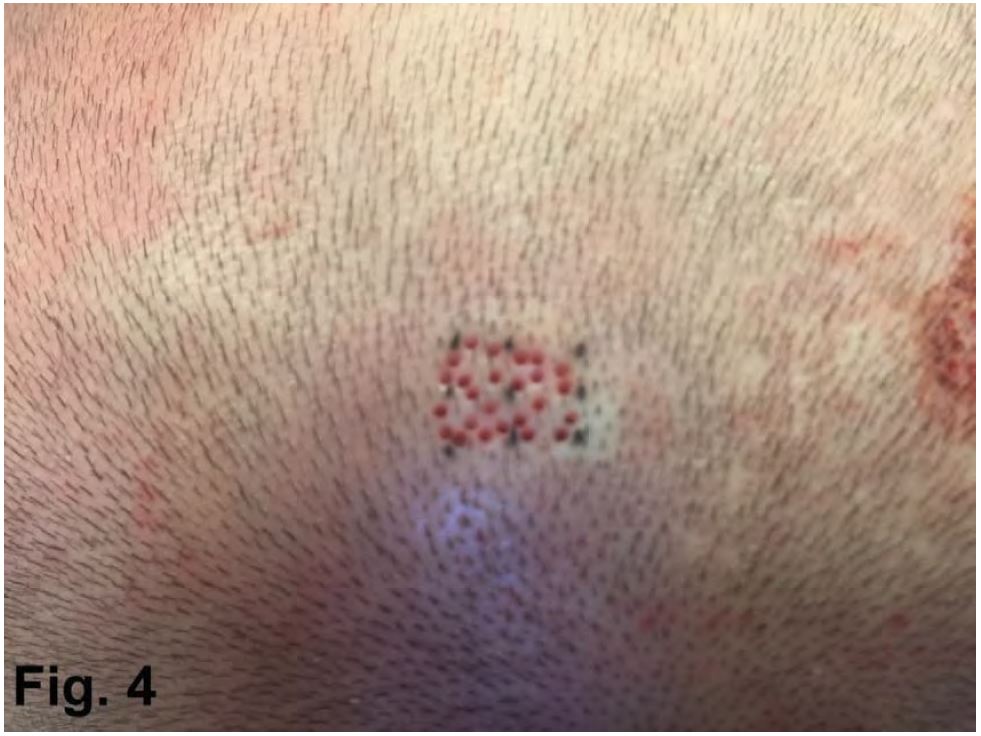
A 0.6 sharp circular punch was used to deliberately increase the transection rate while harvesting within the marked areas. (Fig 4)
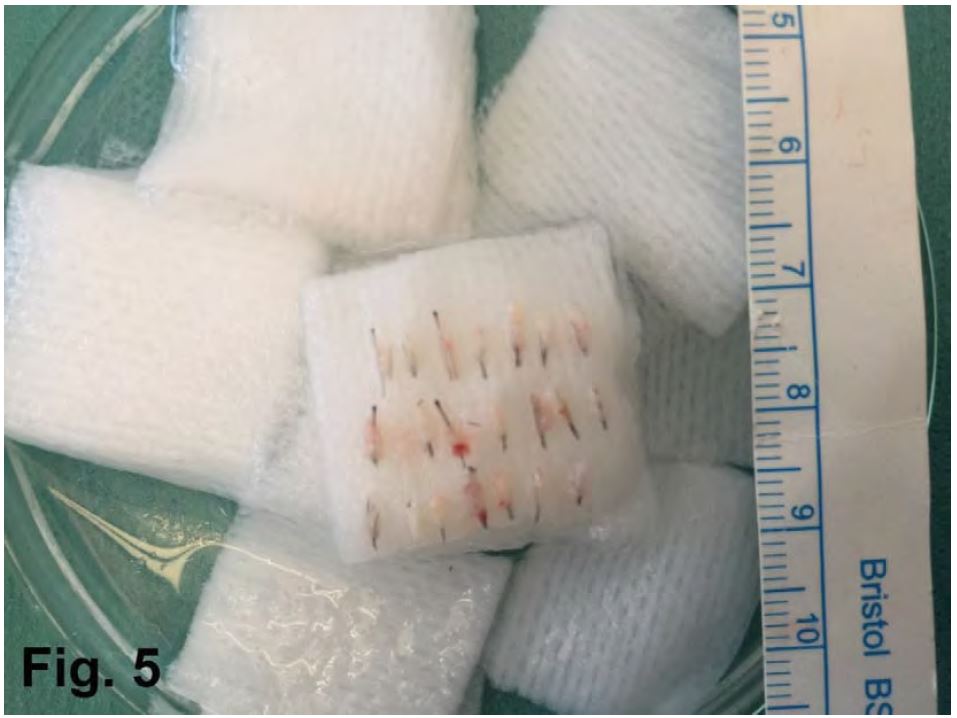
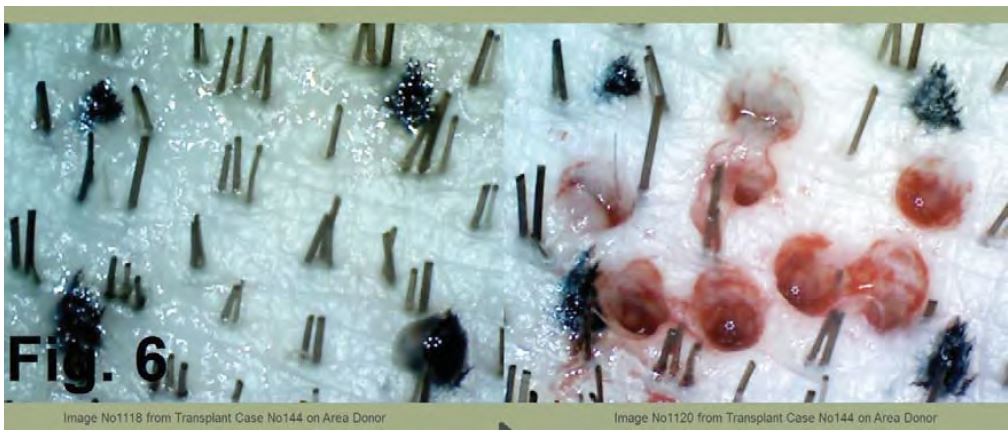
 The remaining FUs were photographed whereas the extracted grafts were photographed and observed under astereoscope, (Fig 5,6)
The remaining FUs were photographed whereas the extracted grafts were photographed and observed under astereoscope, (Fig 5,6)
 Therefore, the following parameters were recorded for each square
Therefore, the following parameters were recorded for each square
- Number of harvested grafts
- Number of intact FUs
- Number of intact hair follicles
- Number of transected hair follicles
- Number of totally transected FUs
- Number of baby hairs which are not visible to the naked eye
The patient returned after 7 months and the hair within the marked areas were trimmed to 1-2mm following micro-photographs were taken of each square respectively.
Results
The statistical analysis of all the data was performed using SPSS version 19. Statistically differences were considered significant at p<0.05. On average, the hair count before and after 7 months shows that the transected follicles have regenerated at 84% (regeneration rate ranges from 43% to 100%). Thus, the regeneration growth depends on the level of transection. Furthermore, partially transected follicular units have had a better regrowth from the totally transected FUs.
Conclusion
The hypothesis that the transected follicles regenerate normally is validated for some FUs but not for all of them.Our study proves that the transected follicles potentially regenerate at high rates. However, it has been proved that high transection rate may affect the vitality of the remaining part of the transected follicles. This probably depends on the level of the follicle where the transection occurred.
Therefore, high transection rate can potentially damage a certain portion of the remaining follicles which may have significant cosmetic and practical consequences to the donor area in FUE harvesting.
Scalp Micropigmentation: an Effective Means to Cover Baldness?
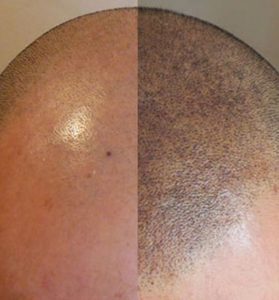 In addition to medical and surgical hair loss treatments, the appearance of baldness can be reduced cosmetically by decreasing the contrast between the scalp and hair using hair loss concealers like Toppik or DerMatch. However, these types of concealers are temporary and can be felt when touching the hair, which can be embarrassing. Scalp Micropigmentation (SMP) is a medical tattoo used as a permanent or long-lasting baldness concealer. The procedure has enjoyed a surge in popularity in recent years and is offered by many high-profile hair restoration clinics and dedicated SMP clinics.
In addition to medical and surgical hair loss treatments, the appearance of baldness can be reduced cosmetically by decreasing the contrast between the scalp and hair using hair loss concealers like Toppik or DerMatch. However, these types of concealers are temporary and can be felt when touching the hair, which can be embarrassing. Scalp Micropigmentation (SMP) is a medical tattoo used as a permanent or long-lasting baldness concealer. The procedure has enjoyed a surge in popularity in recent years and is offered by many high-profile hair restoration clinics and dedicated SMP clinics.
Despite its popularity, there are those that question its ability to reproduce a long-lasting, natural appearance. Dr. Sunil Mishra of Mumbai, India studied 35 patients with baldness who underwent SMP using black and brown inks in order to determine if the procedure is safe a safe and effective means of covering baldness cosmetically.
Results and Conclusion
Dr. Mishra concluded that baldness was effectively treated cosmetically with Scalp Micropigmentation. Patients with hair transplant strip scarring, vertex pattern androgenic alopecia, traumatic scars and female pattern hair loss were very satisfied with micropigmentation in improving their baldness. Hair transplant density results were effectively augmented with the help of SMP.
Scalp Micropigmentation can be used as a good alternative to treat baldness cosmetically. Also, it adds to the armamentarium to help achieve satisfactory outcomes after hair transplant in severe grades of baldness.
Meeting Summary
Thanks to the dedication of skilled and experienced hair transplant surgeons and other hair loss professionals, hair restoration (both medical and surgical) has continued to grow and advance. Our thanks to those physicians who attended this year’s ISHRS meeting in Prague and contributed to the writing of this presentation.
—-
Pat, Bill and David – The Hair Restoration Team for the Hair Transplant Network, the Coalition Hair Loss Learning Center, and the Hair Loss Q & A Blog.